TTAV is experiencing heavy censorship on many social media channels since we’ve been targeted by the mainstream media sellouts, social media bullies, and political turncoats. Be sure to get the TRUTH by subscribing to our email list. It’s free.
![]()
The human papillomavirus (HPV) vaccine was originally approved by the U.S. Food and Drug Administration (FDA) in 2006, and was introduced to the public as a vaccine that could protect women against the two strains of the HPV virus, HPV 16 and HPV 18, believed to be responsible for 70% of all cases of cervical cancer.1
At the time that the vaccine was introduced, the HPV virus, which, according to professionals, is a sexually transmitted infection, was said to have infected approximately 80% of women in the U.S. However, according to research, there are in fact more than 100 strains of this virus, the majority of which are not serious and can clear up on their own without any medical intervention.2,3
Although the HPV vaccine is often referred to as the cervical cancer vaccine, it is debatable whether or not this vaccination can in fact prevent cervical cancer. In 2006, the year that the HPV vaccine was approved for use in the U.S., the American Cancer Society estimated that a total of only 9,710 new cases of cervical cancer would be diagnosed.4
However, despite these facts being widely available, the HPV vaccination is now regarded by many to be one of greatest vaccinations ever developed. Maybe the reason for this is the fact that the HPV vaccination is being falsely portrayed as a vaccine that can protect women against cervical cancer. This may just be because the World Health Organization (WHO) has stated on their website that:
Human papillomavirus (HPV) causes cervical cancer, which is the fourth most common cancer in women, with an estimated 266,000 deaths and 528,000 new cases in 2012. A large majority (around 85%) of the global burden occurs in the less developed regions, where it accounts for almost 12% of all female cancers.” 5
We believe that this statement is extremely misleading because it gives the impression that all women who contract the HPV virus will automatically develop cervical cancer which, according to our research, is completely untrue.
However, we believe that the claim on the U.S. Centers for Disease Control and Prevention (CDC) website was even worse, because the CDC stated:
Protect Your Daughters from Cervical Cancer
Cervical cancer was once the leading cause of cancer deaths among women in the United States. Thanks to HPV vaccine and cervical cancer screening, it is the most preventable of all of the female cancers.”6
Once again, according to our research, their information appears to be completely untrue, because, in 2006, the year that this vaccine was approved, the American Cancer Society had predicted that more women would die from ovarian and breast cancer than from cervical cancer.6
Many Believe that False Claims by the Media are Misleading Parents
With leading health authorities like WHO and the CDC making these sorts of claims, it is easy to understand why the HPV vaccine is being portrayed by many advertising companies as the cervical cancer vaccine, as opposed to a vaccine to protect individuals from the HPV virus.
Over the years, many people have come to believe that in order to boost sales of the vaccine, the pharmaceutical industry and the media have made a number of false claims when advertising the HPV vaccination.

At the time, many believed that the advert gave parents the false impression that if their daughter received the HPV vaccine, the vaccine would protect her against cervical cancer for life.
Having researched the vaccination in depth and knowing that the information given on these advertisements was incorrect, I decided that this particular advertising campaign was a step too far. It was for this reason that I decided to make a stand and complained to the Advertising Standards Authority (ASA). I stated that there was no evidence to support that Cervarix could protect children against cervical cancer for life, and backed my complaint with as much evidence as possible.
At the time of my complaint, I included a letter to my local Member of Parliament, Mr. Nick Gibb, who, at that time, was the Shadow Minster for Education. Mr. Gibb subsequently wrote to the ASA himself to complain.
After many months of letter writing, I eventually received the following letter:
Parents Complain about Merck’s Gardasil Vaccination Advertising Campaign
However, when it comes to the HPV vaccination, GlaxoSmithKline was not the only pharmaceutical company to use emotive language to push vaccination sales. Merck took their advertising campaign for the Gardasil vaccination to a whole new level.
In their adverts, Merck used young actors and actresses to pretend that they have developed cancer from the HPV virus. This is a tactic that many people believe is being used by Merck to guilt trip parents into having their children vaccinated.8
As if this level of deception is not bad enough, Merck then encouraged the actors and actresses to look straight into the camera and ask their parents whether or not they knew that the HPV vaccine could have protected them against the HPV virus that caused them to develop cancer.
This was executed when each actor asked the following question: “Did you know? Mom, Dad?”
You can watch the Merck ad here.
Despite Widespread Use of the HPV Vaccine, Cervical Cancer Rates Are On the Rise
However, despite the increase in the numbers of youngsters receiving the vaccine, according to research, it appears that instead of the rates of cervical cancer decreasing, as one would expect, the rates of cervical cancer have increased dramatically.
In April 2018, Lars Anderson published a paper titled Increased incidence of cervical cancer in Sweden: Possible link with HPV vaccination.9
He stated that:
The Centre for Cervical Cancer Prevention in Sweden has noted in its annual report a substantial increase in the incidence of invasive cervical cancer, especially during the two years 2014 and 2015. I have sub-grouped the data according to age, using the same statistical database of the National Board of Health and Welfare as used by the authors of the above-mentioned report. The increase in the incidence of cervical cancer was shown to be most prominent among women 20–49 years of age while no apparent increase was observed among women above 50.”
Throughout his paper, the data suggested that since the HPV vaccination was approved in 2006, the incidence of cervical cancer had risen significantly, from a total of 202 cases in 2006, to a total of 317 cases in 2015.
To explain this increase further, Anderson gave several possible explanations. He stated that:
A change in the routine or other technical or methodological changes during the study period may affect the reported incidence of cervical cancer due to changes in the sensitivity of the diagnostic tools. The reported change in the incidence among younger women and the fact that the increase was noted in most counties in Sweden argue against this explanation. Neither was such an explanation given by the NKCx in its annual report of 2017, with data up to 2016. Recently, when the Swedish media discussed the increase in the incidence of cervical cancer, the health authorities were unable to explain the increase.”
He continued:
Another possibility is that HPV vaccination could play a role in the increase in the incidence of cervical cancer. About 25% of cervical cancers have a rapid onset of about 3 years including progression from normal cells to cancer. Therefore, an increase may be seen within a short period of time. Gardasil was approved in Sweden in 2006. In 2010, the vaccination of a substantial number of girls started. In 2010, about 80% of the 12-year-old girls were vaccinated. Combined with 59% of the 13–18-year-old girls vaccinated through the catch-up programme in the same period, one can say that most girls were vaccinated. Thus, the oldest girls in the programme were 23 years old in 2015; and this is well within the younger age group shown in Fig. 1. For the older age group represented in Fig. 1, data on exposure to vaccinations is not available. In 2012–2013, most young girls were vaccinated.”
However, we believe that Anderson made his feelings about the HPV vaccination abundantly clear in his conclusion. He wrote:
Could the HPV vaccination cause an increase in invasive cervical cancer instead of preventing it among already infected females and thereby explain the increase in the incidence of cancer reported by the NKCx in Sweden? The increased incidence among young females, the possibility of virus reactivation after vaccination, the increase in premalignant cell changes shown by the FDA for women who were already exposed to oncogenic HPV types and the time relationship between the start of vaccination and the increase in cervical cancer in Sweden could support this view. The answer to this question is vital for correctly estimating the benefit-risk of this vaccine. More studies focused on already HPV-infected individuals are needed to solve this question.” (own emphasis)
Sadly, since his paper was published in April 2018, the paper has been retracted. The Indian Journal of Medical Ethics stated that, the reason they retracted this paper was because: “…. The author gave his name and affiliation as Lars Andersson, department of Physiology and Pharmacology, Karolinska Institutet (KI), Sweden. On May 8, as soon as KI informed us that no such person worked there, we carried out a correction on the same day and the institution’s name was removed as affiliation.”
Further Studies Prove that the Rates of Cervical Cancer Have Increased
Despite Anderson’s paper being retracted, however, Anderson was not alone in his findings. In December 2018, James Lyons-Weller published an article titled HPV Vaccine and Cervical Cancer Rates: UK 1995-2015, in which he highlighted similar findings to those of Anderson.10
Lyons-Weller began his article with the following statement:
Vaccination against the human papillomavirus is supposed to reduce the risk of cervical cancer. Introduced in 2006, we were told that the full effect of the vaccine on cervical cancer rates in the young women vaccinated against HPV won’t be known until the patients in those studies reach the age of 45-50, which is around the year 2050.” (own emphasis)
We believe that the clue to what he has discovered lies in the word “supposed.” He stated that:
Cancer Research UK, the agency that tracks cervical cancer rates in the UK, provides easily accessible cervical cancer incidence data online. Using their data, I calculated the percent change in cervical cancer in three age groups, relative to the rates in 1995.”
He wrote:
It is problematic why, if the HPV vaccine is supposed to reduce the risk of cervical cancer risk, the data show the opposite for the age cohorts who have thus far received the vaccine.” (own emphasis)
To explain his findings in more depth, Lyons-Weller used a series of charts, taken from the Cancer Research UK website.11
He stated that:
The first likely contributing factor for this near-doubling increase in cervical cancer risk in women aged 20-34 is that medical doctors believe, and therefore tell, their patients that they are protected “against HPV” infection. In reality, the vaccine only targets nine types of HPVs, and there exist over 150 other types, many of which are rarer, and are associated with cancer.”
He continued:
The second likely contributing factor is the decision that people make when their doctors tell them that they are immune to an STD; people may take on a riskier sexual lifestyle, including increasing the number of partners, or having more frequent unprotected sexual encounters with new sexual partners.”
To conclude, Lyons-Weller recommended that the following steps should be taken by both the government and the medical profession to ensure that patients have a better understanding of the vaccinations capabilities and are therefore better protected against the HPV virus:
Clearly, the message that people receiving the HPV vaccine are protected “against HPV” has to be modified to “only protected against the vaccine types”, and the message that the vaccine will “reduce cervical cancers” must be accompanied by “if additional steps are taken to protect oneself against infection by non-vaccine targeted HPV types. Also, cervical cancer screening with Pap smears must continue to be recommended. Pap smears are a curative diagnostic and women should be encouraged to begin Pap smears at an early age.”
It appears that James Lyons-Weller is 100% correct, because, according to the Cancer Research UK website, the rates for cervical cancer are predicted to rise significantly by the year 2035.12
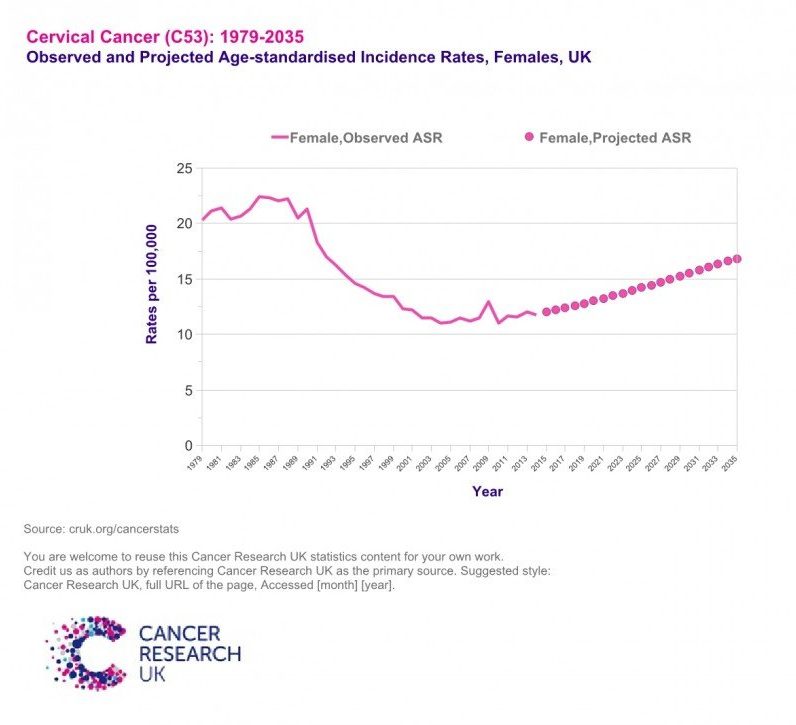
The Evidence Just Keeps on Coming
In September 2018, an article on Changing Times, an independent journalism website, stated that, according to French orthopedic surgeon, oncologist, and statistician Gérard Delépine, the HPV vaccination was certainly not reducing cervical cancer and, in fact, the vaccination was responsible for making matters worse.13
Delépine told journalist Annette Gartland that: “In several countries, cervical cancer rates have increased since HPV vaccination was introduced.” He stated:
Studies should be carried out immediately to find out why these increases are occurring. This is a public health catastrophe that necessitates an urgent rethink about HPV vaccination policies.”
And he went on to explain to reporters that:
The biggest increases are among young women aged 18 to 26, the age group which there is the highest vaccination rate.
These increases come after steady decreases in incidence in the years before HPV vaccination began.”
According to the report, Delépine had told reporters that, in the countries where he had studied, where the uptake of the vaccination was high, their official statistics showed an increase in the incidence of invasive cervical cancer. This increase appeared to be three to five years after the start of the vaccination program and, according to him, was affecting only the age groups in which there was the highest vaccination rate.
These are strong words from Delépine and his evidence is indeed worrying because, if he is correct, then once again, this proves that the HPV vaccination is not what it is has been made out to be.
Follow, Subscribe, & SHARE:
1. X, Formerly known as Twitter: https://twitter.com/TTAVOfficial
2. Telegram: https://t.me/TheTruthAboutCancer_Vaccines
3. GAB: https://gab.com/TyCharleneBollinger
4. GETTR: https://gettr.com/user/cancertruth
5. TruthSocial: https://truthsocial.com/@TheTruthAboutCancer
6. CloutHub: https://app.clouthub.com/#/users/u/TheTruthAboutCancer
7. Bitchute: https://www.bitchute.com/channel/vX3lcHH4Dvp0/
8. Rumble: https://rumble.com/c/TheTruthAboutCancerOfficial
9. Brighteon: https://www.brighteon.com/channels/thetruthaboutcancer










As a Mom, I made the decision years ago to not give my children the HPV vaccine. Something about it just didn’t ‘sit right’ with me. And I had heard stories (although unverified by myself) about the vaccine causing infertility and even death. I only have one daughter and I didn’t want her to suffer from infertility the way I did.
After reading this article I am even more grateful for my ‘Mom senses’ helping me protect my children. I teach them abstinence, the only 100% sure way to protect yourself from STD’s. Think that’s naive in this day? I can give you thousands of examples of young people who will tell you it’s not only possible but makes life happier.
Thank you for your mission to bring us the TRUTH about cancer and vaccines!!!!
Wishing you and your family many blessings, Jane!
Very good article. I think there should be a followup discussing the very high rate of adverse reactions and deaths from these vaccines. So it is not only that the vaccines are causing increased rates of cervical cancer, but they are killing and maiming girls boys upon vaccination. What a double whammy! Just go to the NVIC site for case histories of vaccine damaged and killed girls.
Thank you Christina for your unrelenting research and expose of the false promises of this often devastating vaccine.
My Doctor highly recommended the Gardasil vaccines for my daughter. I had personally dealt with Cervical cancer on more than one occasion. He said this would help her not to contract it and drew me a diagram of how it helps to keep the uterus clean. My daughter suffered greatly after receiving the Gardasil vaccine.
For the next few years. I was made to believe that my daughter was sudden suffering from depression , which she was not, to making me believe that she was somehow suffering from anxiety, which she was by then, thinking she was going crazy, to even being given shots for non existent allergic reactions.
She began to turn blue at swim competitions, and not being able to stand after finishing her events. A Doctor friend of mine, in internal medicine, whose child swam as well, referred us to a pediatric cardiologist at Emory. My daughter had POTS syndrome!
The anxiety that all of this cause my daughter, and the loss of a college scholarship, because she couldn’t participate anymore was devastating for her. She went from an outgoing leader, swim teacher, lifeguard, team Captain, to struggling to keep her chin up.
I just don’t understand why this is allowed to happen, and why a company has no responsibility to the injuries they cause to innocent children!
My 13 year old has developed Scoliosis in a very short time since receiving this Vaccination along with three other girls that we know of in her grade.
Germany has done a study and found 10% of vaccinated girls end up with Scoliosis compared to 0% of unvaccinated girls.
Not sure where to start in our fight to be heard.
Hi Melanie, we’re sorry to hear that your daughter was injured by vaccines.
Unfortunately, the amount of money that pharmaceutical companies are pumping into our medical industry and government have left us with a broken system in which vaccines are not adequately tested and in which manufacturers cannot be sued when their products result in injury or death.
However, there is a program called the Vaccine Injury Compensation Program (VICP) that hears cases regarding vaccine injury. To date, the VICP has paid out over $4 billion to victims. This is your best, if only, recourse when seeking compensation for injury. You can learn how to file a claim here: https://www.hrsa.gov/vaccine-compensation/how-to-file/index.html. The battle is not over, however, and as we continue to keep the national conversation about vaccine safety going, we continue to gain ground slowly but surely. Check out this recent article about an expert witness who was misrepresented during VICP hearings: https://thetruthaboutcancer.com/vaccines-and-autism/. He recently submitted an affidavit stating that there may be a subset of children who are at risk for ASD regression if they have underlying mitochondrial dysfunction and are exposed to vaccines.
There is hope for change in our broken medical industry as long as we continue to ask questions and refuse to stay quiet.
Hope this helps! Wishing you blessings and love!
My 12 old daughter has just been put forward for this vaccine in the UK.
Someone kindly shared your article. I had almost certainly decided not to let her have it but wanted to arm myself with information to back up my decision, your information is extremely helpful.
Whilst on my search I have come across a man whose daughter has been badly affected by the vaccine. Is the link for reporting injuries just for US citizens?
Also am I right in thinking that Lars Anderson’s paper was removed because they added an extrax ‘s’?
Many thank for sharing the information in the article.
Well done, for speaking out. The ‘clinical trial’s were not real… relying on a non inert placebo, and used only half the aluminium adjuvant that is in the ‘approved’ vaccine injected into children, globally, unwittingly. HPV vaccines are a modern scandal with deaths and harms in over 50 Countries – highlighted by the most harmful reported effects from ANY vaccine, not limited to: chronic fatigue, premature menopause, heart irregularity, seizures, paralysis, appendix removal, vomiting and constant nausea. See Youtube for sad cases, post HPV vaccination.
I agree that pharmaceutical marketing in the US is unethical and that big pharma uses manipulative language to attract customers. However, I do need to point out the irony of you using a wealth of manipulative language in this article to encourage people not to vaccinate. In this case,you are the equal, but opposite, to big pharma and the truth lies somewhere in between your manipulative language and their manipulate language.
I’m distrustful of the pharmaceutical industry, but I’m equally distrustful of the anti-vaxx community.
• Good morning. (Thank you for all your information that you are providing for the truth About Cancer and other important health information.)
• In Australia last night 4.3.2019 there was a talkback show on Radio station “triple M,” Australia, and the presenter Luke Bona had a woman come on in response to his topic of whether anti-vaccine people should be stopped from advertising and saying anything on Facebook or other sites, and although he did ask whether it was a case of “freedom of speech,” but because in his opinion vaccinations are “be all that ends all,” (virtual panacea:)
• The woman caller was stating her opinion on vaccines, and he just strongly came out and said I don’t agree with you, and we don’t want any of this virtual rubbish or lie, put out or on his show, and rudely cut her off and hung up on her, whilst continuing to say “in his opinion” and spoke about, and mentioned as an example of poliomyelitis when he was young, and he mentioned that apparently he had some children at his school in calipers.
• And went on to state and claim that going on past years and centuries, as his example to current situations, he states that vaccinations save lives.
• If, as he states his earlier question, of one of the topics to the listeners for talkback was the topic of “does freedom of speech count;” well there was certainly no “freedom of speech” on his particular radio program, because as soon as somebody has a differing opinion to him he straightaway cuts them off and hangs up on them, with negative comments about those people.
~~~~~~~~~~~~~~~~
• I thank you for your very good work that you are doing in your quest, worldwide.
Hi Brian – thanks so much for your comment. This is terrible to hear. And you’re absolutely right about freedom of speech. It’s clear that most platforms don’t even allow freedom of speech on this matter and it’s absolutely shocking.
Absolutely agree that while these findings are very important to know and make the world aware of, there needs to be another addressing the maming and deaths from these HPV vaccines.
Hi Darci, thank you for your comment. We are working on a follow-up article coming soon. Stay tuned!
I understand that there was also censorship of people who opposed the US invasion of Iraq. There has been a very dangerous trend in the 21st century.
While everyone is entitled to their own opinion and are anti-vaccine, to begin with. What I did not see mentioned here is that HPV 16 is a huge cause of throat cancer in men and women both. My late husband and I were told by his oncologist that it can lie dormant like many herpes viruses, shingles for example for many many years. When my late husband was diagnosed with Stage 4 cancer with HPV16 as the cause in the base of his tongue, right tonsil and right lymph none, he was a strong healthy 62-year-old man of 6’1″ and 255 lbs. By the time he was done with the first round of radiation and chemo that did kill off all of that, he was at around 180 lbs. We got him back up to around 190 and he was feeling pretty well when it came back into the lining of his left lung making it inoperable, untreatable and therefore terminal. Apparently, it was already throughout his body when they found it the first time. By the time I lost him 6 months later he was down to about 138 lbs. Yes, at first we were told to vaccinate our daughters, then we were told to vaccinate our sons because they can be carriers and accidentally transmit it to the wives, girlfriends or partners and later we were told to vaccinate our sons because they can actually contract cancer from HPV16 also! This all needs to be mentioned when talking about this vaccination. Maybe the cervical cancer rates are still going up but HPV16 in one of the largest and fastest-growing causes of throat cancer now too. So maybe this vaccine can save someone from going through what I did to a cancer that my wonderful husband contracted long before he’d even met me!!!!
Thank you so much for sharing your experience with us, Ginny. We’re so sorry to hear about your lovely husband. We’ll be sure to keep you in our prayers and wish you endless comfort, love, and support. ❤️
My son got injured by the HPV vaccine. We always have been totally pro vaccination, which has completely changed now. They advertise for their vaccines like car dealers, and many people do just believe this BS – like me. I’ve studied physics and chemistry – and was not aware that pharmaceutical scientists are NO scientists at all. Now I know!
This is the story of my son:
https://hpv-vaccine-side-effects.com/the-hpv-vaccination-can-cause-very-serious-side-effects-2/
my mom developed cervical cancer a year after she was vaccinated.